By FnF Correspondent | PUBLISHED: 20, May 2021, 11:36 am IST | UPDATED: 24, May 2021, 20:41 pm IST
As India struggles with a deadly second wave of Covid-19, cases of a rare fungal infection called “mucormycosis” have been reported in several states. Also known as black fungus, the life-threatening disease has infected many Covid-19 patients including those who have recovered.
Although it is not yet classified as an outbreak, as the number of cases continues to grow, here is what you need to know: What is mucormycosis or black fungus and what causes it? Mucormycosis is an infection caused by a fungus called mucormycete present in the environment. Extremely rare fungal infection has potentially fatal infection starts in the nose and spreads to the eyes and then the brain.
Public health experts are blaming the indiscriminate use of steroids to treat COVID-19 as the likely cause. Steroids reduce inflammation in the lungs. But overuse of these drugs in COVID-19 patients can result in lowered immunity and raised blood sugar levels. These conditions leave some patients, particularly those with uncontrolled diabetes, susceptible to such infections.
What is the black fungus?
Mucormycosis is an invasive infection caused by a class of molds called mucormycetes. These fungi are ubiquitous, naturally occurring in our environment, most commonly in soil. Humans get the infection by inhaling the fungal spores floating around in the air and in dust. These spores get lodged in the nasal passages and sinuses and cause disease at that site.
But not everyone exposed to the spores will get the infection. For most part, if you have a normal immune system, it’s an asymptomatic, silent encounter. But developing the invasive disease depends on a person’s health condition.
People with compromised immune systems, for example, those with blood cancer undergoing chemotherapy or bone-marrow transplant patients who can’t form neutrophils—a type of white blood cell that defends against infections—in the initial weeks, may fall victim to mucormycosis.
Steroids can cause blood sugar levels to spike, which can be especially challenging for patients with uncontrolled diabetes. Higher blood sugar levels and more acidic blood creates a fertile environment for Mucorales fungi to thrive.
In such vulnerable patients, the spores germinate to form long tubular filaments that can grow into the sinuses, into the bone, and the blood stream. The symptoms of mucormycosis and progression of the infection can vary from person to person; they include a throbbing headache, fever, facial and nasal pain, blackish nasal discharge, loss of vision, toothache, loosening of teeth, swelling in the upper jaw, and sometimes face paralysis.
Symptom
* Sinusitis — nasal blockage or congestion, nasal discharge (blackish/bloody)
* Local pain on the cheekbone, one-sided facial pain, numbness or swelling
* Blackish discolouration over the bridge of nose/palate
* Loosening of teeth, jaw involvement
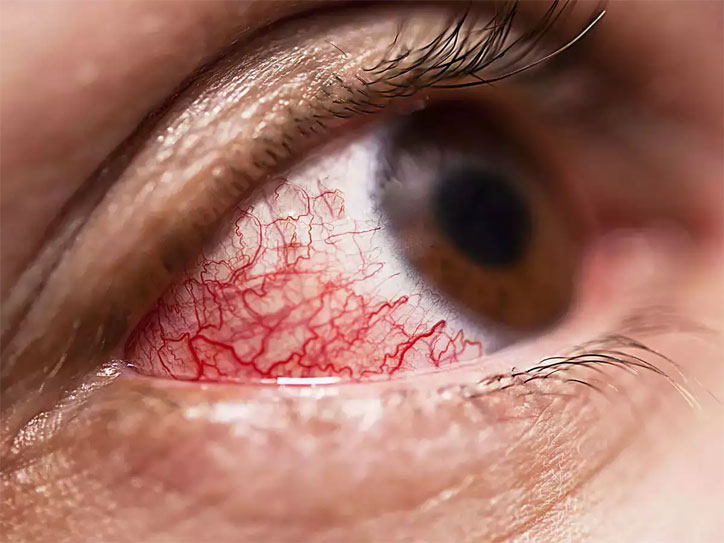
* Blurred or double vision with pain
* Thrombosis, necrotic skin lesion
* Chest pain, pleural effusion, worsening of respiratory symptoms
Mucormycosis can affect different parts of the body, showing different sets of symptoms, according to the CDCTrusted Source.
If the infection grows in the sinuses and brain (rhinocerebral mucormycosisTrusted Source), symptoms include fever, one-sided facial swelling, headache, and nasal or sinus congestion.
If your lungs are affected by the fungus, you can experience cough, chest pain, and shortness of breath.
When mucormycosis attacks the digestive system, you may experience abdominal pain, nausea and vomiting, and gastrointestinal bleeding.
“It’s an environmental mold, which once it infects you, is very morbid and has a high mortality,” said Dr. Eric Cioe-Peña, director of Global Health at Northwell Health in New York. “Because the infection is so rare, the exact mortality rate isn’t clear. But researchers estimate that overall, 54 percent of people with mucormycosis die.”
He added that people with COVID-19 theoretically could be at higher risk due to an immune reaction, or inflammation locally in the sinus tract. Cioe-Peña confirmed the fungus isn’t normally contagious.
According to Bhayani, you can contract the fungus by inhaling the mold spores or when you come into contact with them in things like soil, rotting produce or bread, or compost piles.
“Mucormycosis is normally not spread person to person, but is found in the environment,” he said.
Who’s at risk and how is mucormycosis treated?
According to researchersTrusted Source, while mucormycosis is comparatively rare, increased use of chemotherapy and steroid drugs — like those used to treat some COVID-19 patients — may be increasing its frequency.
In a recent small studyTrusted Source, scientists concluded that COVID-19 patients with diabetes that were treated with steroid drugs had a significantly increased risk of experiencing fungal infections like mucormycosis.
According to Dr. Nikhil Bhayani, infectious disease expert at Texas Health Resources, mucormycosis can be treated with antifungal agents like amphotericin B, isavuconazole, and posaconazole.
“In severe cases, your doctor may recommend surgery to remove infected or dead tissue to keep the fungus from spreading,” he said. “This might include removing parts of your nose or eyes. This could be disfiguring, but it’s crucial to treat this life threatening infection.”

by : Priti Prakash
The year 2025 dawned with New Delhi gazing lovingly into the mirror of its own expectations. After a...